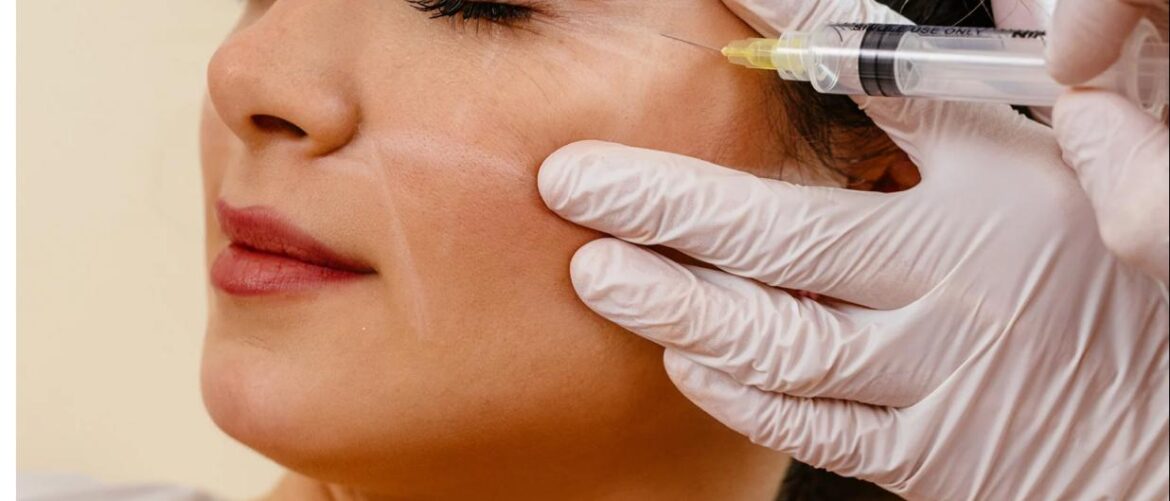
Managing Periorbital Tearing and Double Vision After Botulinum Toxin Type A
 Faramarz Rafie MD / Vancoderm Academy and College (VDA) / Vancoderm Clinic (VDCMed)
Faramarz Rafie MD / Vancoderm Academy and College (VDA) / Vancoderm Clinic (VDCMed)
Botulinum toxin type A
Botulinum toxin type A is a highly purified neurotoxin that has become a cornerstone in both cosmetic and therapeutic medicine. In aesthetic practice, it is most commonly used to soften dynamic facial wrinkles—including crow’s feet, glabellar lines, and forehead rhytids—by temporarily inhibiting acetylcholine release at the neuromuscular junction, leading to controlled muscle relaxation. Beyond its cosmetic applications, BoNT-A is clinically indicated for a variety of medical conditions, such as primary hyperhidrosis, chronic migraine prevention, blepharospasm, and cervical dystonia, reflecting its versatility in modulating neuromuscular activity safely and effectively.
Indications– Crow’s Feet
Botulinum toxin type A is indicated for cosmetic reduction of lateral periorbital lines (crow’s feet) and is appropriate for patients who seek non-surgical facial rejuvenation. Specific indications include:
-
Dynamic rhytids at the lateral canthal region
-
Mild to moderate periorbital lines
-
Patients seeking non-surgical rejuvenation to improve facial aesthetics
Medical note: BoNT-A is most effective for dynamic wrinkles caused by repeated muscle contraction, rather than static lines caused by dermal thinning.
Contraindications
BONT-A injections require careful patient assessment to avoid complications. Contraindications are classified as absolute and relative.
 Absolute Contraindications
Absolute Contraindications
-
Known hypersensitivity to botulinum toxin or any excipients
-
Active infection at the proposed injection site
-
Neuromuscular disorders: e.g., myasthenia gravis, Lambert-Eaton syndrome
-
Pregnancy and breastfeeding
-
History of angioedema or severe allergic reactions to neurotoxins
Relative Contraindications (Caution Required)
-
Age considerations: patients <18 years or >75 years require careful dosing
-
Concurrent medications that interfere with neuromuscular transmission (aminoglycosides, curare-like agents)
-
Previous facial surgery or trauma affecting injection sites
-
Pre-existing eyelid or orbital disorders, e.g., ptosis, entropion, or dry eye syndrome
Definition of Adverse Effects
Epiphora (Excessive Tearing)
Epiphora is the abnormal overflow of tears onto the face, caused either by overproduction of tears or obstruction/dysfunction of the lacrimal drainage system. In the context of Botulinum toxin type A treatment, epiphora most often occurs due to unintended diffusion of the toxin to the orbicularis oculi muscle or lacrimal gland, which can disrupt normal tear drainage and trigger reflex hyperlacrimation.
Clinical significance: Patients may experience ocular irritation, blurred vision, social discomfort, or chronic tearing, making early recognition and management essential for both safety and patient satisfaction.
Diplopia (Double Vision)
Diplopia is defined as the simultaneous perception of two images of a single object, resulting from misalignment of the eyes caused by extraocular muscle weakness or paralysis. In aesthetic Botulinum toxin type A procedures, diplopia can occur if the toxin diffuses into adjacent extraocular muscles (commonly the lateral rectus or superior oblique), leading to temporary paresis and impaired ocular motility.
Clinical significance: Diplopia can affect visual function, depth perception, and daily activities such as reading or driving. While typically transient, it can cause significant patient distress and requires prompt clinical assessment.
Etiology of Tearing (Epiphora) and Double Vision (Diplopia) After Botulinum toxin type A
While Botulinum toxin type A is generally safe when administered by trained professionals, periorbital injections can occasionally result in epiphora or diplopia due to unintended diffusion of the toxin. Understanding the underlying mechanisms is critical for prevention, management, and patient counseling.
1. Epiphora (Excessive Tearing)
Pathophysiology:
Epiphora after Neurotoxin injections typically arises from altered function of the orbicularis oculi muscle, lacrimal gland, or lacrimal drainage system, leading to impaired tear drainage or reflex hypersecretion. Key mechanisms include:
- Diffusion to the lacrimal gland – BoNT-A may reduce sympathetic innervation, paradoxically increasing tear production.
- Orbicularis oculi weakness – Over-relaxation of the lateral or lower eyelid muscles can prevent effective tear pumping into the lacrimal puncta.
- Mechanical factors – Pre-existing eyelid laxity, lower lid malposition, or prior eyelid surgery can exacerbate tear overflow when periocular muscles are weakened.
Predisposing factors:
- High-dose or superficial injections near the lateral canthus
- Inadequate anatomical landmark identification
- Pre-existing tear duct obstruction (dacryostenosis)
- Older patients with lax eyelid structures
2. Diplopia (Double Vision)
Pathophysiology:
Diplopia after Botulinum toxin type A results from temporary paresis of extraocular muscles due to inadvertent toxin diffusion beyond intended injection sites. This causes ocular misalignment, leading to binocular diplopia.
Mechanisms include:
- Diffusion to extraocular muscles – Lateral rectus or superior oblique muscles are most commonly affected.
- Injection technique errors – Excessive dose or incorrect needle placement increases the risk.
- Altered neuromuscular transmission – The neurotoxin temporarily inhibits acetylcholine release at the neuromuscular junction, weakening ocular muscles.
Predisposing factors:
- High-dose lateral periocular injections
- Thin orbital septum or advanced age
- History of strabismus or orbital surgery
- Anatomical variations in orbital musculature
Management and Follow-Up of Neurotoxin-Induced Epiphora and Diplopia
Effective management of Neurotoxin-related tearing (epiphora) and double vision (diplopia) requires a systematic, evidence-based approach to ensure patient safety, minimize complications, and maintain treatment satisfaction.
Immediate Management
Patient Reassurance
- Most cases of epiphora or diplopia are transient, typically resolving within 2–12 weeks as the effect of the neurotoxin diminishes.
- Educate patients regarding the expected timeline of recovery, emphasizing temporary functional impairment to reduce anxiety.
- Ophthalmology Consultation
- Persistent or severe diplopia warrants urgent referral to an ophthalmologist or neuro-ophthalmologist.
- Assessment should include ocular motility evaluation, visual acuity, binocular alignment, and fundus examination to rule out underlying pathology.
Symptomatic Relief
Epiphora: Use lubricating artificial tears or ocular gels to improve comfort and reduce irritation.
Diplopia: Temporary measures such as prism glasses or eye patching may be employed to alleviate visual discomfort during the recovery period.
Monitoring and Follow-Up
- Schedule weekly to biweekly follow-ups for the first 4–6 weeks post-injection.
- Document severity, progression, and patient-reported symptoms at each visit.
- Assess whether future Botulinum toxin type A sessions require dose modification or altered injection sites to prevent recurrence.
- Use clinical documentation to inform risk assessment and patient counseling for subsequent treatments.
Preventive Measures
Preventing these adverse effects is crucial in medical aesthetics practice:
Anatomical Accuracy
- Perform detailed pre-injection mapping of the lateral canthus, orbital rim, lacrimal gland, and extraocular muscles.
- Avoid diffusion of neurotoxin into structures responsible for tear production or ocular motility.
Conservative Dosing
- Use the lowest effective dose in periocular regions, especially in elderly patients or those with thin orbital septa.
- Employ microdroplet techniques or diluted formulations when treating sensitive areas.
Injection Technique
- Maintain adequate distance from the orbital rim and lacrimal gland.
- Use appropriate needle length and angle to limit deep diffusion.
Consequences of Improper Management
Failure to identify and manage these complications can lead to:
-
Persistent ocular discomfort and social inconvenience from excessive tearing.
-
Temporary functional impairment such as difficulty reading, driving, or performing fine visual tasks.
-
Decreased patient confidence in aesthetic procedures and clinician competence.
-
Rare but serious outcomes: Repeated technical errors may contribute to permanent ptosis, prolonged diplopia, or chronic tear dysfunction.
 About Vancoderm Academy & College:
About Vancoderm Academy & College:
As a leader and pioneer in medical aesthetics education in Canada, Vancoderm Academy & College is committed to providing evidence-based, hands-on training for future aesthetic practitioners. Our next intake for the Clinical Practitioner Specialist Diploma in Medical Aesthetics is scheduled for April 1, 2026.
We sincerely thank you for following our updates and supporting our community. Stay connected with us on Instagram, LinkedIn, and Facebook to receive the latest news, educational tips, and professional insights from Vancoderm.