Hemosiderin Pigmentation: Insights, Mechanisms, and Advanced Treatment Strategies
 FARAMARZ RAFIE MD / VANCODERM ACADEMY AND COLLEGE (VDA) / VANCODERM CLINIC (VDCMED)
FARAMARZ RAFIE MD / VANCODERM ACADEMY AND COLLEGE (VDA) / VANCODERM CLINIC (VDCMED)
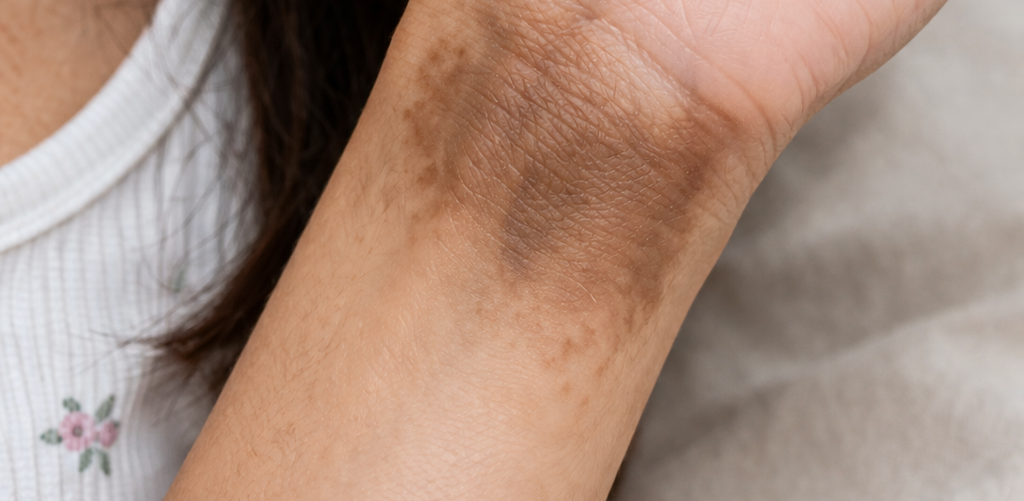
This week’s blog by Vancoderm Academy and College focuses on hemosiderin pigmentation. I recently evaluated a client presenting with localized hyperpigmentation on the left wrist, resulting from intravenous iron supplementation administered four months ago, likely due to extravasation and subsequent iron deposition in the surrounding tissue.
Definition
Hemosiderin pigmentation refers to a localized discoloration of the skin caused by the accumulation of hemosiderin, an iron-storage complex derived from the breakdown of hemoglobin. This results in a brownish or yellow-brown hyperpigmentation, often observed in areas of previous trauma, inflammation, or vascular compromise.
Reasons
Hemosiderin deposition in the skin occurs when iron accumulates in the dermis, leading to persistent hyperpigmentation. Several factors can contribute to this condition. Chronic venous insufficiency, often seen in the lower extremities, causes blood pooling and red blood cell breakdown, releasing iron that is subsequently stored as hemosiderin in the skin. Repeated trauma, bruising, or hematomas can similarly result in localized iron deposition. Hemorrhage, whether due to injury or medical conditions affecting coagulation, can also contribute to pigment accumulation. In the context of intravenous iron therapy, extravasation—or leakage of the iron-containing solution from the vein into surrounding tissues—can trigger localized hemosiderin pigmentation. The severity and extent of pigmentation depend on factors such as the concentration of iron, duration of tissue exposure, and the patient’s skin type and vascular integrity. Additional contributing factors may include inflammation, slow lymphatic drainage, or repeated injections at the same site, which increase the likelihood of iron retention in the dermis.
Mechanism
Hemosiderin pigmentation results from the deposition of iron-containing compounds in the dermis, primarily as a consequence of red blood cell breakdown or direct extravasation of iron. When red blood cells are damaged or extravasated, hemoglobin is released into the surrounding tissue. Macrophages phagocytose this hemoglobin and metabolize it into hemosiderin, an insoluble iron-storage complex. Hemosiderin accumulates within dermal macrophages and the extracellular matrix, causing a characteristic brownish or yellow-brown discoloration of the skin. The depth of deposition can vary, with superficial dermal accumulation producing lighter, more diffuse pigmentation, while deeper dermal storage results in more persistent and darker lesions. The severity and persistence of pigmentation are influenced by several factors, including the total amount of iron introduced or released, the duration of tissue exposure, local vascular integrity, and the patient’s ability to mobilize and clear iron through normal lymphatic and enzymatic pathways. Chronic inflammation or repeated trauma at the site can exacerbate iron deposition, prolonging pigment retention and making spontaneous resolution slower.
How to Treat (Hemosiderin Pigmentation)
Treatment of hemosiderin pigmentation focuses on promoting the clearance of iron deposits from the dermis rather than inhibiting melanin production. Topical retinoids, such as retinol or tretinoin, are effective because they enhance epidermal turnover, stimulate dermal remodeling, and facilitate gradual removal of hemosiderin-laden macrophages. Antioxidants, including Magnesium Ascorbyl Phosphate (MAP), reduce oxidative stress and support collagen synthesis, aiding tissue repair and improving skin tone.
For persistent or deep dermal pigmentation, procedural interventions are often required. Microneedling and radiofrequency-assisted microneedling mechanically stimulate the dermis, enhancing turnover and pigment clearance. Chemical peels may assist with superficial pigment removal but are less effective for deeper deposits.
Laser therapies provide an important complementary option for improving results. Q-switched lasers are designed to deliver short, high-energy pulses that target pigment particles, breaking them into smaller fragments that can be removed by the body’s lymphatic system. PicoWay, a picosecond laser platform, offers a similar mechanism with even shorter pulse durations, minimizing thermal damage to surrounding tissue while effectively targeting hemosiderin deposits. These laser platforms can accelerate pigment clearance, especially for stubborn or longstanding lesions, and are often used in combination with topical therapies for optimal outcomes.
Treatment selection depends on the depth and severity of pigmentation, the patient’s skin type, and response to previous therapies. Multiple sessions may be required for deep dermal pigmentation, and a combination of topical and procedural approaches generally provides the best results.
Magnesium Ascorbyl Phosphate (MAP) – Formulation and Mechanism in Pigmentation Management
Magnesium Ascorbyl phosphate (MAP) is a stable, water‑soluble derivative of vitamin C created by esterifying ascorbic acid with magnesium. Unlike pure ascorbic acid, which is inherently unstable and prone to rapid oxidation when exposed to air, light, or heat, MAP is significantly more stable in cosmetic and dermatological formulations. This enhanced stability allows products to maintain efficacy over longer shelf life and reduces the likelihood of irritation, making MAP a preferred form of vitamin C in dermatological use, especially for patients with sensitive or compromised skin.
Once applied topically, MAP penetrates the stratum corneum and is enzymatically converted to active ascorbic acid within the skin. This conversion allows it to exert the beneficial effects of vitamin C while minimizing the irritation commonly associated with high concentrations of pure ascorbic acid.
Mechanisms of Action Relevant to Pigmentation:
Tyrosinase Inhibition:
MAP inhibits tyrosinase, the key enzyme in melanogenesis (melanin production). By reducing tyrosinase activity, it limits the synthesis of melanin at its source, which helps reduce the formation of new pigment and gradually fades existing hyperpigmentation.
Antioxidant Activity:
As a potent antioxidant, MAP neutralizes reactive oxygen species (ROS) produced from UV exposure and inflammation. Oxidative stress upregulates melanocyte activity; by reducing ROS, MAP lowers melanocyte stimulation, which helps prevent further pigmentation.
Collagen Support and Dermal Repair:
The active ascorbic acid generated from MAP supports collagen synthesis by acting as a co‑factor for prolyl and lysyl hydroxylase enzymes. Enhanced collagen production fortifies dermal structure, improving skin texture and reducing post‑inflammatory pigment retention by normalizing repair processes.
Anti‑Inflammatory Effect:
Vitamin C derivatives, including MAP, modulate inflammatory cytokines. Since inflammation can exacerbate melanogenesis through post‑inflammatory hyperpigmentation (PIH), reducing inflammation indirectly limits pigmentation formation.
Advantages of MAP Compared to Other Vitamin C Forms:
- Greater stability in aqueous formulations
- Lower irritancy potential (useful for sensitive skin or compromised barriers)
- Effective tyrosinase inhibition with sustained delivery
- Compatible with a broader range of pH environments (unlike pure ascorbic acid, which requires low pH for stability)
Expected Timeframe for Visible Improvement
The time required to observe noticeable improvement in hemosiderin-induced hyperpigmentation depends on multiple factors, including the depth of iron deposition, the chronicity of pigmentation, the patient’s skin type, and the treatment modality used.
For topical therapies, such as magnesium Ascorbyl phosphate (MAP), hydroquinone, retinoids, or vitamin C formulations, initial lightening of pigmentation may be visible after 6 to 12 weeks of consistent daily use. Maximum improvement often requires 3 to 6 months, particularly for deeper dermal pigmentation, because the turnover of pigmented dermal macrophages and gradual removal of hemosiderin is a slow biological process.
For procedural interventions, including chemical peels, laser therapy, or Microneedling, improvement may be seen more quickly, often within 2 to 4 weeks after the first session for superficial pigment, but deeper pigmentation usually requires multiple sessions over 2 to 6 months. The combination of topical and procedural approaches can accelerate clearance but still requires patient compliance and protective measures, such as broad-spectrum sunscreen, to prevent re-pigmentation.
Chronic or longstanding lesions, especially those resulting from repeated iron extravasation, may take several months to over a year for near-complete resolution. Complete removal is sometimes not achievable, and treatment aims to significantly lighten pigmentation and improve cosmetic appearance rather than guarantee full clearance.
To Care
Post-treatment care is a critical component of managing hemosiderin pigmentation and ensuring optimal results from both topical and procedural therapies. The affected area should be protected from UV exposure at all times, using a broad-spectrum sunscreen with SPF 30 or higher. Sun protection is essential even on cloudy days or indoors near windows, as UV radiation can trigger inflammation and prolong pigment retention.
Gentle skin hygiene should be maintained to avoid irritation. Use mild, non-abrasive cleansers and avoid exfoliants, scrubs, or aggressive mechanical treatments that could disrupt healing. Moisturizing daily helps restore and maintain the skin barrier, supports dermal repair, and reduces inflammation, which can otherwise contribute to slower pigment clearance.
Patients should avoid trauma or friction at the treatment site, including tight clothing, scratching, or pressure, which could exacerbate hemosiderin retention. For areas treated with procedures such as Microneedling, laser therapy, or chemical peels, it is important to follow professional instructions regarding cleansing, application of healing ointments, and interval between sessions.
Topical therapies, including retinoids such as retinol or tretinoin and antioxidant serums like Magnesium Ascorbyl Phosphate, should be applied as directed. These agents help promote epidermal turnover, stimulate dermal remodeling, and support gradual removal of hemosiderin deposits.
Hydration and a balanced skincare routine are important for enhancing skin recovery and preventing additional pigmentation. Patients should also monitor the treated area for signs of irritation, prolonged redness, or infection, and report any concerns promptly to the clinician. Regular follow-up appointments allow the practitioner to assess progress, adjust treatment protocols, and reinforce preventive strategies to minimize recurrence.
there are several recent and clinically relevant updates in how hemosiderin‑related hyperpigmentation (especially from iron extravasation) is understood and treated. These refinements come from dermatology and aesthetic medicine research and reflect a better understanding of pigment biology, treatment mechanisms, and outcomes. Here are the key medical developments:
1. Clear Distinction Between Melanin vs Iron Pigmentation
Recent consensus in dermatologic practice emphasizes that hemosiderin pigmentation should not be treated with melanin‑targeted agents (like hydroquinone). Because the pigment originates from iron breakdown products — not melanin — treatments must focus on promoting dermal clearance of iron and dermal remodeling rather than inhibiting melanin synthesis. This aligns treatment with the pathophysiology rather than a generic hyperpigmentation model.
2. Improved Understanding of Laser Interaction with Iron Pigment
Not all pigment lasers are equally effective on hemosiderin. Traditional pigment lasers (e.g., those tuned for melanin) often have limited efficacy against iron complexes. Recent clinical observations highlight that:
- Q‑Switched Nd:YAG lasers (especially 1064 nm) can target deeper dermal pigment without excessive melanin absorption.
- Picosecond platforms like PicoWay deliver ultra‑short pulses that fragment iron deposits more efficiently and with less thermal injury, improving safety and reducing post‑inflammatory pigmentation risk.
- Combining wavelengths (e.g., alternating 1064 nm with 532 nm where appropriate) may enhance clearance across superficial to deep dermal layers.
Published case series now support multiple pass, low‑fluence protocols to maximize pigment fragmentation while minimizing dermal trauma.
3. Adjunctive Pharmacologic Modulation of Iron Metabolism
Emerging research suggests topical agents that affect local iron metabolism may enhance pigment clearance. These include:
- Iron chelators: Compounds such as deferoxamine can bind free iron. Experimental studies and limited clinical use show potential to reduce iron load when applied topically under controlled conditions.
- Antioxidant combinations: Products combining vitamin C derivatives with niacinamide, azelaic acid, or green tea polyphenols may reduce oxidative stress induced by iron deposits and support repair processes more effectively than single‑ingredient formulations.
4. Role of Dermal Macrophage Dynamics
Newer insights from dermatopathology emphasize that the persistence of hemosiderin pigment depends on the efficiency of macrophage clearance and lymphatic transport. Treatments that improve lymphatic flow — such as gentle manual lymphatic drainage or low‑level laser therapy — may theoretically support pigment resolution, though evidence remains limited and mostly observational.
5. Combination Treatment Protocols Show Better Outcomes
Standalone topical or procedural therapies often yield partial improvement. Multiple recent clinical reports suggest the best outcomes come from strategic combination protocols, such as:
- Initial laser sessions to physically break up dermal deposits
- Follow‑up with topical retinoids + stable vitamin C derivatives (e.g., MAP) to enhance turnover
- Periodic Microneedling to improve product penetration and tissue remodeling
This tiered approach appears to accelerate clearance compared with singular modalities.
6. Increased Emphasis on Patient Stratification
Not all patients respond equally. Dermatologists now stratify treatment based on:
- Depth of pigment (epidermal vs dermal)
- Duration since onset
- Skin phototype
- Presence of vascular insufficiency or previous trauma
This results in more personalized plans — for example, deeper pigment may prioritize laser, whereas very recent superficial deposition might respond better to topical regimens initially.
7. Refined Expectations and Counseling
Clinical experience supports a more nuanced understanding of time to improvement:
- Early lightening might occur within 4–6 weeks with combination therapy
- Significant improvement generally takes 3–6 months
- Some deep, longstanding lesions may persist beyond 12 months and require maintenance therapy
Counseling now emphasizes that complete pigment elimination is not guaranteed and that treatment aims for visible reduction and cosmetic enhancement rather than full clearance.
 continues to stand as a leader and pioneer in innovative, medically and academically oriented medical aesthetic education in Canada. Our comprehensive Clinical Practitioner Specialist Diploma in Medical Aesthetics is designed to equip students with the knowledge, skills, and hands-on experience required to excel in the field. The next intake is scheduled for April 1, 2026, and applicants are encouraged to secure their spots early. We sincerely thank our readers for their continued support and for following us on Instagram, LinkedIn, and Facebook, and we wish you all the very best in your educational and professional journey.
continues to stand as a leader and pioneer in innovative, medically and academically oriented medical aesthetic education in Canada. Our comprehensive Clinical Practitioner Specialist Diploma in Medical Aesthetics is designed to equip students with the knowledge, skills, and hands-on experience required to excel in the field. The next intake is scheduled for April 1, 2026, and applicants are encouraged to secure their spots early. We sincerely thank our readers for their continued support and for following us on Instagram, LinkedIn, and Facebook, and we wish you all the very best in your educational and professional journey.
See you Next Week!