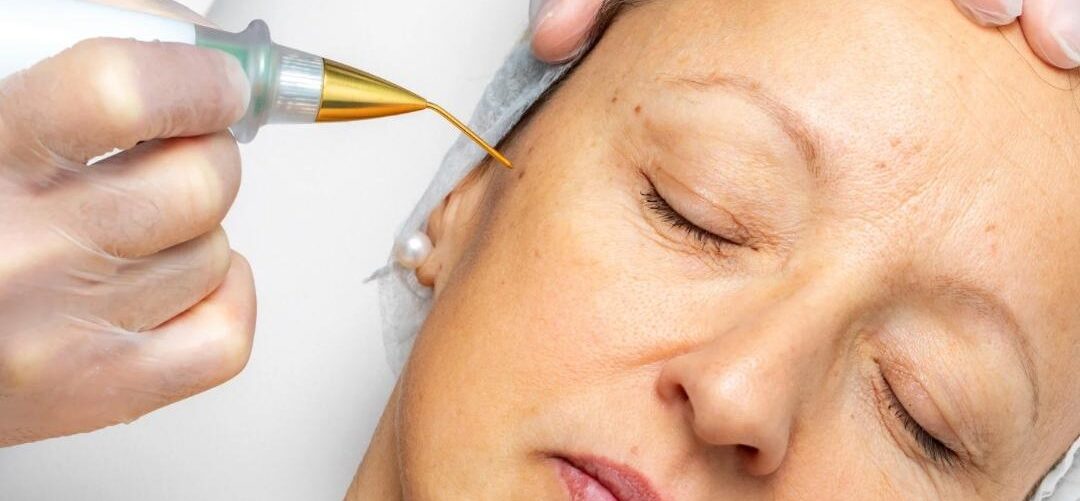
Plasma Laser Treatments: The Future of Non-Surgical Skin Rejuvenation
Faramarz Rafie MD / Vancoderm Academy and College (VDA) / Vancoderm Clinic (VDCMed)
Plasma Laser Treatments: The Future of Non-Surgical Skin Rejuvenation
In the rapidly evolving field of medical aesthetics, plasma laser technology has become one of the most in-demand innovations for non-surgical skin tightening and advanced skin rejuvenation. At Vancoderm Academy in Vancouver, BC, we emphasize results-driven, evidence-based training that prepares students and practitioners to confidently perform high-demand treatments. Plasma laser therapy represents a powerful combination of precision, safety, and clinical effectiveness—making it a cornerstone in modern aesthetic practice.
Understanding the Mechanism of Plasma Laser Technology
Unlike conventional laser systems that rely on light amplification, plasma devices generate ionized gas (plasma energy) through a high-voltage difference between the device tip and the skin surface. This interaction produces a controlled micro-arc that leads to a process known as sublimation.
Key Mechanisms Involved:
- Sublimation Effect:
The plasma arc causes instant conversion of solid epidermal tissue into gas without passing through a liquid phase. This creates precise micro-injuries on the skin surface while minimizing thermal diffusion to surrounding tissues. - Thermal Stimulation:
Controlled heat is delivered to the dermal layers, inducing collagen denaturation and contraction, which results in immediate skin tightening. - Fibroblast Activation:
The micro-trauma stimulates fibroblast cells, triggering neocollagenesis (new collagen formation) and elastogenesis (elastin production), improving skin structure over time. - Wound Healing Cascade:
The body initiates a natural repair response involving growth factors, cytokines, and tissue remodeling, leading to progressive skin rejuvenation over several weeks.
This multi-layered biological response is what makes plasma laser treatments highly effective for long-term skin improvement.
Types of Plasma Laser Devices in Medical Aesthetics
 Plasma technologies can be categorized based on their energy delivery systems, intensity, and clinical application:
Plasma technologies can be categorized based on their energy delivery systems, intensity, and clinical application:
1. Fibroblast Plasma Pens (Low to Medium Energy): Advanced Clinical Insights for Non-Surgical Skin Rejuvenation in Vancouver
Fibroblast plasma pens represent a core modality within plasma laser treatments and are extensively utilized in medical aesthetics for non-surgical skin tightening, advanced skin rejuvenation, and fibroblast activation therapy. These low to medium energy devices are highly valued for their precision, controlled tissue interaction, and ability to safely treat delicate anatomical regions such as the periorbital and perioral areas. Their clinical relevance continues to grow in Vancouver, BC, where demand for non-invasive cosmetic procedures is rapidly increasing.
From a biophysical perspective, fibroblast plasma pens function by generating a high-voltage electrical discharge that ionizes atmospheric gases to produce a focused plasma arc. This plasma arc induces controlled epidermal sublimation, resulting in the instantaneous conversion of solid keratinocytes into gas without transitioning through a liquid phase. This mechanism creates precise microthermal injury zones while minimizing lateral heat diffusion and preserving surrounding tissue integrity. Concurrently, localized thermal exposure—typically reaching approximately 60–70°C in the superficial dermis—leads to collagen fiber denaturation and immediate tissue contraction, producing a visible skin tightening effect.
In addition to immediate contraction, the controlled micro-injury initiates a cascade of biological responses central to long-term skin rejuvenation. Fibroblast proliferation is stimulated, promoting neocollagenesis—specifically the synthesis of Type I and Type III collagen—as well as elastin remodeling over a period of 4 to 12 weeks. This regenerative process is further enhanced by the release of growth factors and cytokines, including Transforming Growth Factor Beta (TGF-β), which play a critical role in dermal matrix remodeling and tissue repair.
Technically, fibroblast plasma pens are classified as low to medium energy plasma devices, operating within controlled voltage ranges suitable for superficial to mid-dermal applications. These devices feature adjustable energy outputs to accommodate varying skin thicknesses and treatment indications, along with fine-tip applicators that enable high-precision targeting. The non-contact delivery system significantly reduces the risk of cross-contamination, while specific spot spacing protocols are employed to regulate thermal distribution and optimize healing outcomes. Careful calibration of energy parameters based on anatomical location, treatment goals, and Fitzpatrick skin type (I–VI) is essential for both safety and efficacy.
Clinically, fibroblast plasma pen treatments are indicated for a wide range of cosmetic dermatology concerns, particularly those involving mild to moderate skin laxity and textural irregularities. Common applications include non-surgical blepharoplasty for upper and lower eyelid tightening, reduction of periorbital rhytids such as crow’s feet, and perioral rejuvenation targeting fine lines around the lips. Additionally, these devices are effective in improving superficial atrophic acne scars, reducing static and dynamic wrinkles, and enhancing overall skin firmness and elasticity in localized areas.
The immediate clinical endpoint of treatment is the formation of carbonized micro-crusts, or eschar dots, which indicate precise energy delivery and controlled epidermal injury. These micro-crusts initiate a predictable wound healing response, beginning with an acute inflammatory phase characterized by erythema and edema, followed by crust formation and desquamation typically within 5 to 10 days. Over the following weeks, progressive collagen remodeling occurs, resulting in gradual improvements in skin firmness, elasticity, and texture.
One of the primary advantages of fibroblast plasma pens is their ability to deliver highly targeted treatment with minimal downtime compared to more aggressive ablative laser modalities. They provide a non-surgical alternative for patients seeking skin tightening and rejuvenation without the risks associated with invasive procedures. Additionally, when performed by trained professionals, the risk of deep tissue damage is significantly reduced, making these devices both cost-effective and versatile in clinical practice.
However, due to the thermal and ablative nature of plasma energy, strict adherence to clinical safety protocols is critical. A comprehensive Fitzpatrick skin type assessment is required, particularly because individuals with higher skin types (IV–VI) have an increased risk of post-inflammatory hyperpigmentation. Contraindications must be carefully evaluated, including active infections, a history of keloid formation, uncontrolled systemic conditions such as diabetes, pregnancy, and recent isotretinoin use. Proper pre-treatment preparation—such as skin priming and sun avoidance—and post-treatment care, including infection prevention, UV protection, and maintenance of the skin barrier, are essential to ensure optimal outcomes and minimize complications.
Within advanced aesthetic practice, fibroblast plasma pens occupy a strategic position between superficial cosmetic treatments and more aggressive ablative technologies. They are especially effective for targeted, localized skin tightening where surgical intervention is not indicated. Furthermore, when integrated into a comprehensive treatment plan, plasma fibroblast therapy can be combined with complementary modalities such as chemical peels, Microneedling, and medical-grade skincare to enhance overall clinical results and patient satisfaction.
Overall, fibroblast plasma pens represent a sophisticated and highly effective approach to non-surgical skin rejuvenation, aligning with current industry trends toward minimally invasive, results-driven aesthetic treatments.
2. High-Frequency Medical-Grade Plasma Systems: Advanced Controlled Energy Delivery for Dermal Remodeling
High-frequency medical-grade plasma systems represent an advanced category within plasma energy-based skin rejuvenation technologies, engineered to deliver highly controlled, consistent, and reproducible plasma discharge for non-surgical skin tightening, collagen remodeling, and advanced dermal rejuvenation. These systems are primarily utilized in clinical and medically supervised aesthetic environments due to their increased energy stability, precision targeting capabilities, and deeper tissue interaction compared to handheld fibroblast plasma pens.
From a biophysical standpoint, these systems generate plasma through a regulated high-voltage electromagnetic field, producing ionized gas that forms a stable plasma arc with superior energy uniformity. Unlike lower-tier devices that may produce variable discharge patterns, high-frequency systems maintain consistent waveform output, allowing for predictable thermal distribution and controlled dermal heating. This results in improved procedural accuracy and reduced variability in clinical outcomes.
One of the key advantages of high-frequency plasma systems is their ability to achieve deeper dermal penetration with enhanced precision. The controlled plasma arc induces a more uniform thermal gradient within the epidermis and upper reticular dermis, facilitating targeted collagen denaturation and contraction. This controlled thermal injury stimulates a robust wound-healing cascade, promoting neocollagenesis, elastin fiber regeneration, and extracellular matrix (ECM) remodeling, which collectively contribute to long-term improvements in skin firmness and structural integrity.
Due to their enhanced energy output and depth of action, these systems are typically employed in medical aesthetic clinics, dermatology practices, and advanced training institutions. Their clinical application requires a higher level of practitioner competency, as treatment parameters must be adjusted based on anatomical region, skin thickness, and patient-specific factors such as Fitzpatrick skin type and baseline dermal integrity. Proper energy modulation is essential to avoid excessive thermal accumulation and to ensure controlled tissue response.
In terms of therapeutic outcomes, high-frequency plasma systems demonstrate greater collagen remodeling potential compared to lower-energy plasma devices. This is attributed to their ability to deliver sustained thermal stimulation at controlled depths, resulting in more pronounced dermal contraction and progressive tissue tightening over a 6–12 week remodeling period. This makes them particularly effective for patients presenting with more advanced signs of aging or structural skin laxity.
Given their potency and depth of action, these systems require advanced professional training and strict adherence to clinical safety protocols. Practitioners must be proficient in energy calibration, tissue response recognition, and complication management. Critical safety considerations include precise treatment spacing, thermal threshold control, and comprehensive pre- and post-treatment skin assessment. Additionally, proper infection control measures and patient selection protocols are essential to minimize adverse outcomes such as post-inflammatory hyperpigmentation or thermal injury.
Clinically, high-frequency plasma systems are indicated for moderate skin laxity, deeper rhytids (wrinkles), and advanced skin rejuvenation protocols. They are particularly effective in areas requiring greater structural remodeling, such as the lower face, jawline, and perioral region, where increased dermal support and tightening are required. When integrated into a comprehensive aesthetic treatment plan, they can significantly enhance outcomes in combination with modalities such as resurfacing treatments, collagen induction therapies, and medical-grade skincare regimens.
Overall, high-frequency medical-grade plasma systems occupy a critical role in advanced aesthetic medicine, offering a balance between precision energy delivery and deeper tissue remodeling for patients requiring more intensive non-surgical rejuvenation strategies.
3. Nitrogen Plasma Technology (Plasma Skin Regeneration Systems – PSR): Advanced Controlled Thermal Skin Remodeling
Nitrogen plasma technology represents a more advanced, clinically refined category of plasma-based energy systems used in medical aesthetics for non-surgical skin rejuvenation, dermal remodeling, and advanced collagen stimulation therapies. Unlike conventional fibroblast plasma pens that create focal epidermal injury points, nitrogen-based plasma systems utilize ionized nitrogen gas to deliver uniform, controlled thermal energy across the skin surface without direct epidermal puncture.
From a biophysical and bioengineering perspective, nitrogen plasma is generated when radiofrequency or high-voltage energy ionizes nitrogen gas, producing a stable plasma field. This plasma field delivers consistent, homogenous thermal diffusion to both the epidermis and upper dermis. The absence of direct skin contact or focal arcing allows for a more controlled thermal profile, significantly reducing variability in tissue response and improving procedural safety.
A key distinguishing feature of nitrogen plasma systems is that they produce non-ablative or minimally ablative dermal heating, meaning the skin barrier remains largely intact. As a result, there is typically no formation of open wounds or carbonized crusting, which is commonly observed in traditional plasma pen treatments. This intact epidermal barrier significantly lowers the risk of secondary infection, transepidermal water loss, and prolonged downtime, making it a preferred modality in patients requiring safer, full-field rejuvenation.
The controlled thermal energy delivered by nitrogen plasma induces precise dermal heating within the papillary and upper reticular dermis, triggering a cascade of physiological responses. This includes immediate collagen fiber contraction through heat-induced denaturation, followed by long-term fibroblast activation and extracellular matrix remodeling. Over time, this leads to enhanced neocollagenesis, elastin synthesis, and structural dermal regeneration, which collectively improve skin firmness, elasticity, and overall quality.
Unlike fractional or ablative laser systems, nitrogen plasma technology achieves tissue regeneration without creating open microchannels, which significantly reduces the inflammatory burden on the skin. This contributes to a more predictable healing trajectory and minimizes risks such as post-inflammatory hyperpigmentation (PIH), particularly in higher Fitzpatrick skin types when properly indicated and performed.
Clinically, nitrogen plasma systems are considered highly versatile and are frequently utilized for full-face rejuvenation protocols, offering comprehensive improvement in overall skin quality rather than isolated spot treatment. They are particularly effective in addressing diffuse pigmentation irregularities, fine lines and early rhytides, photodamage, and textural skin concerns. The uniform thermal effect allows for global dermal stimulation, making it suitable for patients seeking overall skin refinement rather than localized correction.
The clinical advantages of nitrogen plasma technology include non-wound-based treatment delivery, reduced infection risk, improved patient comfort, and minimal recovery time compared to traditional plasma modalities. The absence of epidermal disruption also allows for a more controlled post-treatment response, with reduced crusting, lower inflammatory peaks, and more consistent collagen remodeling outcomes.
Despite its favorable safety profile, nitrogen plasma therapy still requires advanced clinical training and precise parameter selection. Practitioners must understand thermal dosing, tissue response thresholds, and individualized treatment planning based on skin thickness, baseline dermal condition, and pigmentation risk profile. Proper patient selection and post-care protocols remain essential to optimize outcomes and ensure predictable regeneration.
In advanced aesthetic practice, nitrogen plasma technology is positioned as a full-spectrum skin rejuvenation modality, particularly effective for improving overall skin texture, mild to moderate laxity, pigmentation irregularities, and fine line correction. When integrated into a structured treatment plan, it may complement other non-invasive modalities such as medical-grade skincare, light-based therapies, and collagen stimulation procedures to achieve comprehensive dermal rejuvenation.
Overall, nitrogen plasma systems represent a significant advancement in plasma-based aesthetics, offering controlled thermal remodeling with enhanced safety, reduced downtime, and superior uniformity in skin rejuvenation outcomes.
4. Fractional Plasma Technology
Fractional plasma technology is an advanced modality within plasma-based medical aesthetics that combines controlled plasma energy delivery with a fractional treatment pattern to achieve targeted skin resurfacing and dermal remodeling. This approach delivers energy in a grid-like or pixelated distribution, treating a fraction of the skin surface while preserving adjacent untreated tissue. The presence of intact surrounding tissue plays a critical role in accelerating re-epithelialization and optimizing wound healing dynamics.
From a physiological perspective, fractional plasma induces microthermal zones of controlled injury across the epidermis and superficial dermis. Each treated microcolumn triggers localized collagen denaturation and initiates a regenerative wound-healing cascade, while the untreated skin islands act as a biological reservoir for rapid cellular migration. This mechanism significantly enhances tissue recovery, resulting in faster re-epithelialization, reduced inflammatory burden, and decreased overall downtime compared to fully ablative approaches.
One of the defining advantages of fractional plasma systems is the ability to customize energy density, pulse duration, and treatment spacing. This allows practitioners to tailor the intensity of dermal injury according to clinical indication, skin thickness, and patient-specific healing capacity. Higher energy settings produce deeper thermal remodeling and more pronounced collagen stimulation, whereas lower settings focus on superficial resurfacing and texture refinement.
Fractional plasma technology is particularly effective in stimulating neocollagenesis and extracellular matrix remodeling. The controlled thermal injury activates fibroblast proliferation and promotes the synthesis of Type I and Type III collagen, leading to progressive improvement in dermal structure over several weeks. Elastin fiber remodeling further enhances skin elasticity and firmness, contributing to long-term rejuvenation outcomes.
Clinically, fractional plasma is widely indicated for acne scarring, where controlled dermal remodeling helps improve atrophic scar depth and surface irregularities. It is also used for textural correction, including enlarged pores, uneven skin tone, and mild surface roughness. In addition, it is effective for mild to moderate aging concerns, such as fine lines, early skin laxity, and photoaging-related changes.
Another significant advantage of fractional plasma is its favorable healing profile. By preserving untreated skin bridges, the technology reduces recovery time and lowers the risk of complications such as prolonged erythema or excessive crusting. This makes it a preferred option for patients seeking clinically meaningful results with manageable downtime.
Despite its safety advantages, fractional plasma treatments still require comprehensive clinical training and precise parameter control. Proper patient selection, Fitzpatrick skin typing, and post-treatment care protocols are essential to minimize risks such as post-inflammatory hyperpigmentation and to ensure consistent treatment outcomes.
Overall, fractional plasma technology represents a highly adaptable and clinically effective approach within plasma-based skin rejuvenation, offering a balance between efficacy, safety, and controlled recovery for a wide range of dermatological and aesthetic indications.
Clinical Advantages of Plasma Laser Technology
- High precision with minimal collateral tissue damage
- Non-invasive alternative to surgical procedures
- Effective for localized treatment areas
- Stimulates natural collagen production without injectables
- Suitable for combination therapies in advanced aesthetic protocols
Safety and Professional Considerations
Due to the thermal nature of plasma energy, proper training is critical. At Vancoderm Academy, students are trained in:
- Fitzpatrick skin type assessment to reduce risk of post-inflammatory hyperpigmentation
- Energy parameter selection based on treatment area
- Infection control and post-treatment care
- Client consultation and contraindications
Plasma laser treatments must always be performed by trained medical aestheticians or qualified professionals to ensure optimal results and patient safety.
Vancoderm Academy is a leading education institute in Vancouver, BC, specializing in advanced training for Medical Aesthetics Diploma programs and professional skin rejuvenation courses, designed to equip students with clinical skills, hands-on experience, and industry-relevant knowledge in modern aesthetic medicine.